Hernández G, Ospina-Tascón GA, Petri Damiani L et al.
JAMA. 2019;321(7):654-664. doi:10.1001/jama.2019.0071
Hypothesis
To determine if a peripheral perfusion-targeted resuscitation (CRT) during early septic shock in adults is more effective than a lactate level-targeted resuscitation for reducing mortality.
Background
Shock is characterised by increasing lactate levels and signs of tissue hypoperfusion. Persistent hypoperfusion is associated with organ failure and increased mortality.
The Surviving Sepsis Campaign traditionally uses lactate to guide haemodynamic resuscitation however there are other causes of a raised lactate. Capillary refill time responds rapidly to fluid resuscitation and is a resource-independent method of assessing tissue perfusion.
Primary Outcome
- All-cause mortality at 28 days
Secondary Outcomes
- Death within 90 days
- Organ dysfunction as per SOFA score after 72 hours of randomisation
- 22 ventilation-free days within 28 days
- RRT-free days within 28 days
- Vasopressor-free days within 28 days
- ICU and hospital length of stay
Tertiary Outcomes
- Total resuscitation fluids during the intervention period;
- Total fluid balance within 8, 24, and 72 hours ;
- Occurrence of intra-abdominal hypertension within 72 hours
- The use of renal replacement therapy within 28 days
- In-hospital mortality.
Cohort and Study Inclusion
28 hospitals in 5 South-American countries (Argentina, Chile, Colombia, Ecuador, Uruguay)
March 2017 – March 2018.
Inclusion criteria:
- ≥18 years with septic shock admitted to ICU
- Septic shock was defined as suspected or confirmed infection + hyperlactatemia (≥2.0mmol/L)
- Needing vasopressors to keep MAP ≥65 after IV fluid 20 mL/kg 1 hour.
- Recruited within 4 hours after fulfilling criteria.
Methods
Intervention period was over 8 hours from the patient being admitted to the ITU.
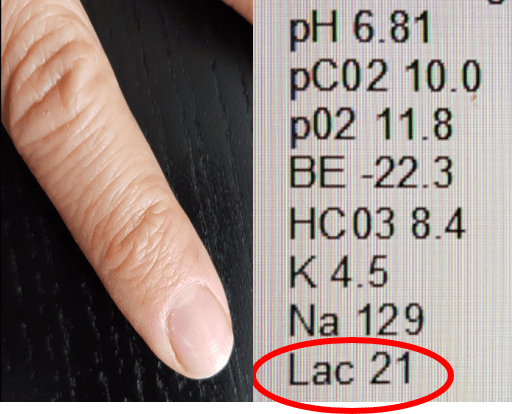
Before commencing study, centres trained and assessed CRT in a standardized method by applying 10 seconds of pressure with a glass microscope slide on distal right index finger. A stop watch was used to measure refill time. A time of >3 seconds was abnormal.
- Lactate level was assessed every 2 hours.
- CRT was evaluated every 30 minutes until normalization. Then measured hourly during intervention period.
- Goals:
- Peripheral perfusion group was to normalize CRT
- The lactate group was to normalize or to decrease lactate levels by 20% every 2 hours.
- Goals achieved by analysing:
- Assess fluid responsiveness.
- 500ml crystalloid fluid challenges every 30 mins
- Either CVP reached or fluid unresponsive
- If fluid unresponsive, resuscitation was continued until goals reached.
- Vasopressors started
- Aim for MAP 80-85 in chronic hypertensive patients
- Measured CRT in 1 hour OR lactate in 2 hours.
- Inodilator test – milrinone/dobutamine
- Measured CRT in 1 hour OR lactate in 2 hours.
- Assess fluid responsiveness.
Statistical Analysis
The study aimed to enrol 420 patients to yield 90% power to detect 28 day reduction in mortality with a prediction that there would be 45% mortality in the lactate group, and 30% mortality in the CRT group. Interim analyses conducted did not show obvious superiority or direct harm, and the trial continued. The study compared resuscitation, perfusion, and haemodynamic variables with Fisher exact tests.
The primary outcome was calculated with Cox proportional hazards adjusted specifically for APACHE II score, SOFA score, lactate level, CRT and infection source. The proportional hazards assumption was tested with the Grambsch and Therneau method. Results are reported as hazard ratio with 95% confidence interval and as Kaplan-Meier curves.
Results
Overall in 424 patients with early septic shock, lactate levels significantly lower at 48 & 72 hours in CRT group than in lactate group p=0.01. CRT values were significantly lower at 4, 8, and 24 hours in the peripheral perfusion group compared with the lactate group P = .01 at 4 hours, P < .01 at 8 hours, P < .01 at 24 hours). However there was no statistical difference at 2, 48 and 72 hours.
Overall 28-day mortality was 34.9% in the peripheral perfusion–targeted resuscitation group compared with 43.4%in the lactate level–targeted resuscitation group, a difference that did not reach statistical significance.
Limitations
- Non blinded study could introduce bias
- Underpowered study to exclude a clinical significance between groups.
- Variability in CRT operator was not analysed
- Randomization not stratified by site and location
- Sepsis protocol based on current guidance and this may change in the future invalidating this study’s methods
- ICU based study which limits its applicability to ward/ED
Conclusion/Discussion
The study concluded that there was no statistically significant difference in 28 day mortality between CRT and lactate targeted strategy.
- The study has a context of heterogenous multinational ICUs
- The study did not specifically assess dangers of fluid overload which influences mortality.
- Septic patients with hypertension should aim for higher MAPS of 80 – this is something that we should be mindful when resuscitating in our own ITU.
- CRT perfused targeted therapy resulted in better SOFA score – in line with observational studies but more research is required in this area.
- CRT has its own issues as it is dependent on age/sex/temperature/light/technique. Age/sex and method were adjusted for by the study however.
Summary by Dr T Gupta. Journal Club Meeting 21 March 2019.