Pinato DJ, Howlett S, Ottaviani D et al.
JAMA Oncology 2019, 2785
Aim of Study
To evaluate whether there is an association between antibiotic therapy administered prior to or concurrently with immune checkpoint inhibitor (ICI) therapy and overall survival and treatment response in patients with cancer treated with ICI in routine clinical practice.
Design and Location
Prospective multicentre cohort study (Imperial College and Chelsea & Westminster)
Methodology
196 patients identified between January 2015-April 2018 who received broad-spectrum antibiotics within a month of starting or during their ICI treatment. Measured overall survival and radiological response to therapy.
Primary Outcome
Overall survival from commencement of ICI therapy.
Secondary Outcomes
Radiological response at 6-8 weeks after commencing ICI therapy using RECIST criteria and without evidence of pseudoprogression
Statistics
Plotted group-specific overall survival using Kaplan-Meier method and tested for between-group difference using the Log-rank test. Uni- and multivariable survival analyses of survival using Cox regression models to evaluate the impact of prior antibiotic therapy on patient overall survival.
Results
Prior antibiotic therapy was associated with worse overall survival (2 months with prior antibiotic therapy vs 26 months without prior antibiotic therapy, hazard ratio 7.4, 95% CI 4.2-12.9 months, p<0.001) and a higher likelihood of primary disease refractory to ICI therapy (81% vs 44% respectively). Independent of tumour site, disease burden and performance status. No statistically significant difference noted in patients receiving antibiotics who are already established on ICI therapy.
Conclusions/Discussions
Receiving broad-spectrum antibiotic therapy in the 30 days prior to starting ICI therapy is associated with worse overall survival and reduced likelihood of radiological response to ICI therapy (presumed to be due to effect on gut microbiome)
Stated Limitations from the Study
Limited sample size and geographical variation
No data on diversity of gut microflora in each patient group
No information on mutational burden of cancers (which may influence prognosis)
Discussion from Journal Club Meeting (?Change of Practice)
- New awareness that prescribing broad-spectrum antibiotics to patients with malignant cancer that is treatment-naïve may affect longer-term outcomes if they could go on to have ICI therapy.
- Prescribing probiotics may become part of routine clinical practice in the future.
- Noted that use of ICI therapy is now routine in multiple metastatic cancer types and that ICI therapy has very different mechanisms of action and therefore side effects compared with other forms of systemic cancer treatment.
Summary by Dr M Taylor. Journal Club Meeting 10 October 2019.
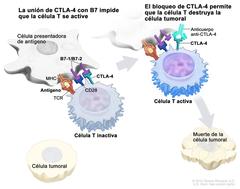
Image from https://visualsonline.cancer.gov/details.cfm?imageid=12204