Cros J, Sengès P, Kaprelian S et al.
Regional Anesthesia and Pain Medicine 2018; 43 (6): 596-604
Aim of Study
Stated hypothesis: Pecs I is superior to multimodal analgesia alone for the treatment of postoperative pain in extended breast cancer surgery.
Design and Location
Randomized, Double-Blind, Dual-Centered Controlled Trial (Montréal, Canada and Limoges, France)
Methodology
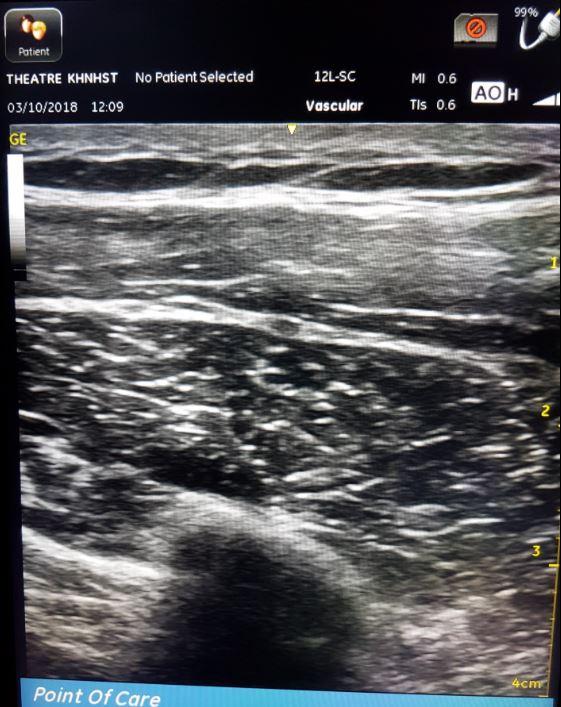
A randomized, double-blinded, dual-centered, placebo-controlled trial was performed. 128 patients scheduled for unilateral breast cancer surgery were recruited. A multimodal analgesic regimen and surgeon-administered local anesthetic infiltration were used for all patients. Ultrasound-guided Pecs I was performed using bupivacaine or saline.
Primary Outcome
Pain score at rest in the post anaesthesia care unit (PACU) 30 minutes after admission or just before morphine administration if the pain score was 4/10 or greater on the numerical rating scale (NRS).
Secondary Outcomes
Pain scores at rest and upon movement (mobilization of the arm on the operated side) using the NRS every 10 minutes in the recovery unit and then every 4 hours on the ward for up to 24 hours for hospitalized patients. Pain scores were recorded 24 hours after surgery for day-surgery patients. Following a phone call at home, pain scores were also recorded by a research assistant at 3 and 7 days after surgery in both patient groups.
The total perioperative sufentanil or fentanyl consumption (in micrograms) was recorded from the anesthesia chart at the end of surgery. Fentanyl doses was converted into the equivalent sufentanil doses (10 μg of fentanyl is equivalent to 1 μg of sufentanil).
The total morphine consumption (in milligrams) was recorded from the recovery nurse records when each patient was discharged from the PACU
The total oral morphine consumption (24 hours after surgery) was recorded after administration on the ward or at home.
The Pecs I complications in the first 24 hours were recorded (eg, bleeding, local anesthetic toxicity, hematoma, motor block, paresthesia, or hypoesthesia experienced in the chest, axilla, or arm).
The cumulative incidences of nausea and vomiting were recorded during the same time frame as the pain scores and were then assessed using a modified 3-point cardinal scale.
Patient satisfaction with pain management was recorded at 24 hours.
The impact of pain on the daily behavior of each patient was assessed using a French version of the brief pain inventory questionnaire, and it was evaluated 1, 3, and 7 days after surgery.
Statistics
The between-group comparisons of the quantitative variables were performed using the Mann-Whitney U test. The normality was assessed using the Shapiro-Wilk test. The between-group comparisons of the qualitative variables were performed using the Fisher exact test.
Results
Primary Outcome: No significant between-group differences in the NRS pain score at rest in the recovery unit after breast cancer surgery (30 minutes after the arrival of the patients in the recovery unit) or just prior to the morphine administration. (bupivacaine: 3.0 [1.0–4.0] vs placebo: 3.0 [1.0–5.0], P = 0.549).
Conclusions/Discussions
Perioperative opioid consumption in the PACU and pain scores up to 24 hours after surgery did not differ between the patients who received a Pecs I block with bupivacaine or saline.
Therefore, the use of a Pecs I block may not be necessary to decrease the pain scores for patients undergoing breast cancer surgery when postoperative analgesia is optimized with dexamethasone, wound infiltration with a long-acting local anesthetic, paracetamol, and NSAIDs ± morphine.
Stated Limitations from the Study
Study was likely underpowered to demonstrate a difference in the primary outcome between the major and minor surgery groups, increased chance of type II error.
Pecs I was performed alone because at the time the protocol was registered, Pecs II had not yet been described.
The patients were only followed up for up to a week; therefore, the risk of developing chronic pain could not be evaluated.
Discussion from Journal Club Meeting (?Change of Practice)
Our practice uses PEC I and II +/- SA block, does this confer additional benefit over PEC I alone?
Local empirical evidence suggests regional breast blocks do significantly improve patient experience, both in terms of pain reduction and reduction of PONV but requires audit of current processes.
Summary by Dr D Wang. Journal Club Meeting 13 December 2018.