Goswami S, Kundra P and Bhattacharyya J.
British Journal of Anaesthesia 2017; 119 (4): 830-83. https://doi.org/10.1093/bja/aex201
Background
It has been demonstrated that PEC2 block provides better quality of analgesia than compared with PEC1 when given pre operatively. Remains to be seen whether the disruption of the interfascial planes after surgery will alter the spread of La and efficacy of PEC1 and PEC2 blocks.
Terms
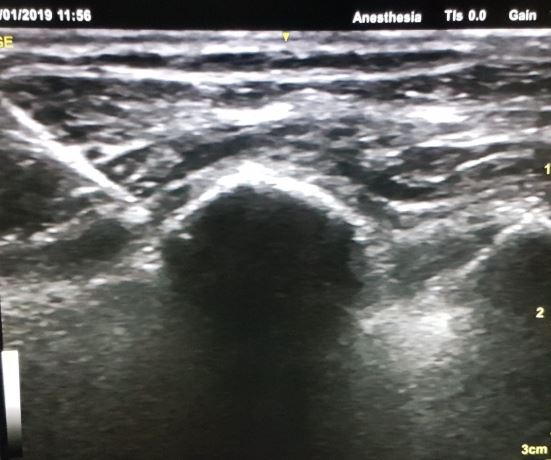
PECS 1 BLOCK: Between Pectoral major and minor. MPEC 2 BLOCK: Between pectoral minor and serratus
Aims
Comparison of PEC1 and Mpec2 blocks as the modality for post op pain relief in patients undergoing modified radical mastectomy.
Primary outcomes
To compare analgesic efficacy of PEC1 and Mpec2 block in terms of;
- time to 1st rescue analgesic,
- VAS Score
- Number of top ups in 24hours
Secondary outcome
To map the spread of sensory block and observe side effects (if any).
Recruitment
- 62 ASA grade I–II female patients 35–65 yr, undergoing unilateral modified radical mastectomy under general anaesthesia were recruited
- Exclusion Criteria:
- Patients with history of hypertension, diabetes, known allergy to local anaesthetic, major cardiac disorders, renal dysfunction, pre-existing neurological deficits, and psychiatric illness
- two patients were excluded from initially recruited 64 patients
Standardisation
- All patients were kept nil orally overnight and premedicated with oral alprazolam 0.25mg and ranitidine 150mg the night before and two h before surgery.
- During the preoperative visit, patient characteristics data was recorded and visual analog scale (VAS; 0–10, 0=no pain, 10=worst pain) was explained to the patients.
Randomisation
- Patients were randomly allocated into two groups (Group PEC1, n=31 and Group mPEC2, n=31)
- The catheter was placed between pectoralis major and minor in Group PEC1 and between pectoralis minor and serratus anterior in Group mPEC2 before wound closure under direct vision by the operating surgeon.
Control of Variables
- 18g Cannula and standard AAGBI monitoring
- General anaesthesia was induced with i.v. fentanyl 1 mg kg1 followed by propofol 1.5–2mg kg1 i.v. until loss of verbal response.
- Tracheal intubation was facilitated with atracurium 0.5mg kg1 and anaesthesia was maintained with isoflurane (minimal alveolar concentration 1–1.3) and 66% nitrous oxide in 33% oxygen through a circle system.
- Patient’s lungs were ventilated with positive pressure ventilation to maintain end-tidal carbon dioxide between 4.0 and 4.5 kPa. ECG, NIBP, SpO2, end tidal carbon dioxide and nasopharyngeal temperature were continuously monitored and recorded throughout surgery.
- All patients received a continuous infusion of ringer lactate solution at the rate of 5–8ml kg1 h1 during surgery.
- Fentanyl 25 mg was given i.v. if mean bp or heart rate exceeded 20% of the preoperative value.
- Any incidence of hypotension (mean arterial pressure< 65mm Hg) was treated with rapid infusion of 200ml ringer lactate and, if required, injection mephentermine was given in 3mg i.v. boluses.
- Bradycardia (HR<50 beats min1) was treated with i.v. atropine (0.6 mg).
- All the patients received ondansetron 0.1mg kg1 i.v. over 20min before completion of surgery.
- At the end of surgery before wound closure, a perforation was made with 18 gauge Tuohy needle just below clavicle and an epidural catheter was passed through it. The surgeon placed the catheter with the tip directed towards axilla, in plane as per group.
- Once the skin closure was completed, 30ml of 0.25% bupivacaine was injected through the catheter under complete aseptic conditions and surgical drains were kept clamped for 15min before making the injection.
- Residual neuromuscular block was antagonized with the mixture of neostigmine (2.5 mg) and glycopyrrolate (0.4mg) i.v. and tracheal extubation was performed when the patient was fully awake.
Post-op
- VAS score measured at 30 minutes, 6, 12, 18, 24 h postoperatively.
- Time for first analgesic top up (primary outcome measure of the study) was noted when the VAS reached>4 or if the patient demanded analgesia.
- Each top up comprised of 15 ml of 0.25% bupivacaine and the number of top ups required in 24h were noted in all patients. If the pain relief was inadequate after a top up dose (VAS score>4), rescue analgesia with 100mg of i.v. tramadol was provided.
- All data was recorded by an investigator who was blinded to the group allocation and was not involved or present during surgery.
Statistical Analysis
- Statistical analysis by Statistical Package
- Authors conducted an initial pilot study of 10 patients
- Sample size calculated on “time to first rescue analgesia”
- Able to estimate required sample size required to detect a difference of 33 minutes
- 80% power
- 5% probability Type 1 Error
Results
- Satisfactory Pain scores in both groups
- Analgesia was significantly prolonged in group mPEC2 [mean(SD)] 313.45(43.05) vs 258.87(34.71)min in group PEC1,P<0.001.
- Total pain experienced over 24h was significantly less in group mPEC2 [mean(SD)] 9.77(6.93) than in group PEC1 24.19(10.81), P<0.0001.
- Consequently, top up requirements were significantly reduced in group mPEC2 than in group PEC1 [median(range)] 3(2-4) vs 4(3-5) respectively, P<0.001.
- Lateral pectoral (77.42% and 35.48%) and thoracodorsal nerves (93.55% and 48.39%) had higher incidence of sensory block in group mPEC2 than group PEC1, P<0.001.
Conclusion
mPEC2 block provides better postoperative analgesia than PEC1 when catheters are placed under direct vision
Summary by Dr J de Bois. Journal Club Meeting 03 January 2019.

Leave a comment